RAISE and 3D organ reconstruction: a project from Spoke 2 with San Martino Hospital in Genoa

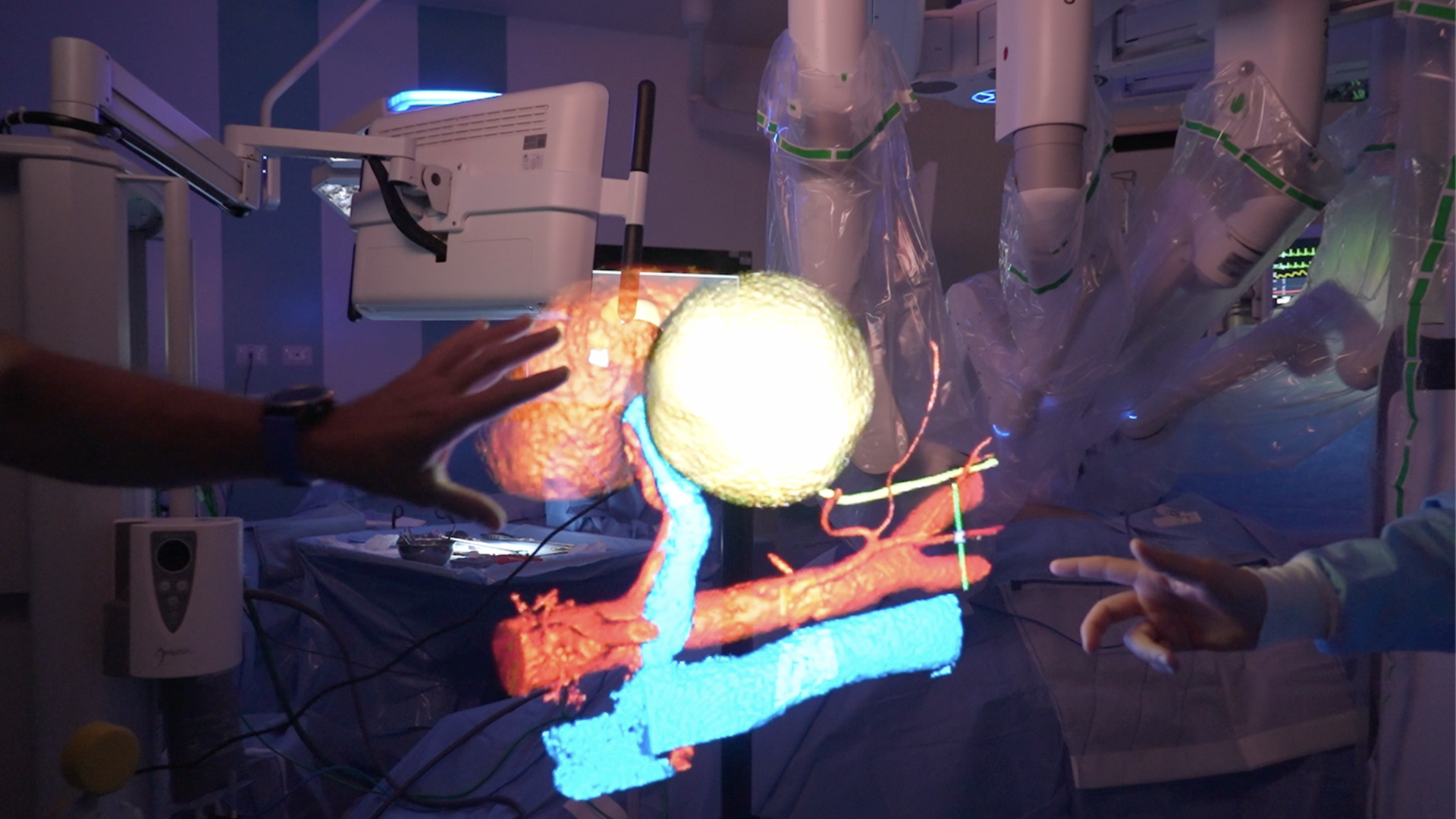
Used in both preoperative and intraoperative planning, these reconstructions significantly improve the quality of patient care and open new avenues for research.
Within the RAISE innovation ecosystem, Spoke 2 – coordinated by Lorenzo De Michieli of the Italian Institute of Technology (IIT) and dedicated to the development of innovative solutions for healthcare, with the support of artificial intelligence and robotics – has launched a flagship project on Advanced Surgical Navigation using 3D organ reconstruction from radiological images. Leading this development is Professor Paolo Traverso, project promoter and coordinator at San Martino Polyclinic Hospital and the University of Genoa.
The San Martino Hospital, along with UniGe’s DISC (Department of Integrated Surgical and Diagnostic Sciences) and DIBRIS (Department of Computer Science, Bioengineering, Robotics, and Systems Engineering), has invested in the clinical testing of this methodology. It has been adopted in daily surgical practice in collaboration with the team led by Professor Carlo Terrone, Director of the Urology Clinic.
This technique enables the creation of digital “twin” organs – highly accurate 3D models faithfully replicating a patient’s anatomy, veins, arteries, and internal structures – using advanced software and holographic projectors. Thanks to these reconstructions, physicians can study anatomical geometry in detail and refine the preoperative strategy, identifying the safest and least invasive surgical path.
“We began using this 3D reconstruction technology from radiological images such as CT scans in 2020,” explained Professor Paolo Traverso. “To date, we’ve completed over 250 reconstructions, used during preoperative and intraoperative phases, which have significantly improved the quality of patient care and opened new research prospects.”
During surgical procedures, the 3D holographic image is integrated with the robotic surgical system, allowing the surgeon to navigate the patient’s anatomy with greater precision. In specific cases, the virtual reconstruction can even be overlaid onto the real surgical field, enhancing visual control and reducing the margin of error in complex procedures such as kidney tumor removal.
“We’ve now brought 3D reconstructions into the operating room,” added Traverso. “Our next goal, supported by PNRR funding through the RAISE project, is to develop intracorporeal navigation, where 3D images are automatically synchronized with the surgeon’s movements, tracking each phase of the operation in real time.”
The project has also demonstrated the technology’s potential in physically reconstructing damaged anatomical parts, such as sections of the jaw or other bones compromised by trauma or tumors. Using digital models, missing fragments can be precisely produced via 3D printing, making reconstructive surgery more accurate, personalized, and effective.
Lorenzo De Michieli, Coordinator of Spoke 2 RAISE, commented on the project: “The results achieved by Professor Traverso’s team represent a key example of the RAISE ecosystem’s innovative potential. The application of 3D organ reconstruction to robotic surgery not only showcases the scientific and technological excellence within Spoke 2, but also paves the way for a fundamental transformation of surgery in the future. These technologies – integrating artificial intelligence, advanced imaging, and personalized 3D models – can decisively contribute to making care more precise, less invasive, and increasingly patient-centered.”
Thanks to the work carried out at San Martino Hospital, the use of 3D reconstruction in Oncological Urology has emerged as both a concrete technology transfer and a clinical innovation, destined to be expanded into other areas of medicine.
